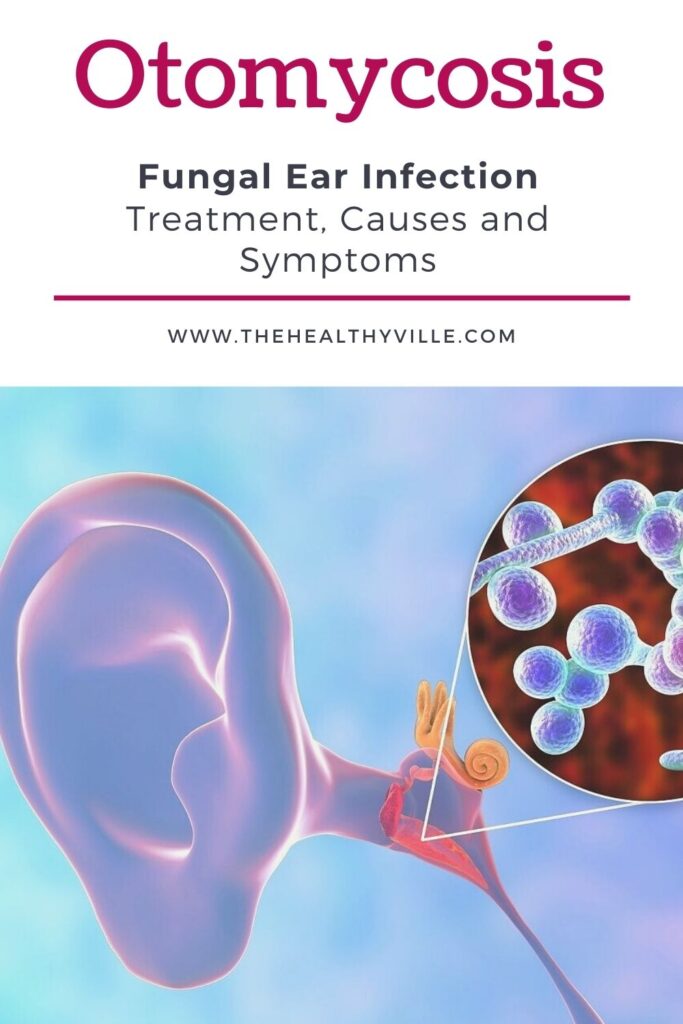
Otomycosis is an infection that happens to the ears. The fungal ear infection treatment options, causes and symptoms are known. Learn more about them!
Otomycosis is an infection of the external auditory canal of an acute and transitory nature. Fungal agents of the genus Aspergillus are the main culprits.
Otomycosis is a fungal infection that frequently settles in the outer ear. It is part of the group of external otitis, but it is not due to bacteria (such as Pseudomonas and other opportunistic pathogens). In this case, the causative agents are the fungi Aspergillus and Candida.
It is estimated that external otitis constitutes 5 to 20% of otological consultations, that is, people who come to the clinic worried about hearing loss and symptoms in the ears. Of all this percentage, less than 20% of the clinical pictures are attributed to fungi. If you want to know everything about this fungal infection, read on.
What is otomycosis?
Fungal external otitis or otomycosis is an infectious disease of the external auditory canal, due to various types of fungi, such as Aspergillus niger. Despite being less common than bacterial otitis, in some temperate and humid regions these events can account for 50% of otic symptoms.
The fungi producing otomycosis depend on the region consulted. Estimations are that the genus Aspergillus responds to 80% of the cases, while the species Aspergillus niger, by itself, causes half of the otomycoses. Behind it are other microorganisms, such as Aspergillus fumigates (30%) or Candida albicans (11%).
These infections take place in the outer ear, especially in the ear canal. This canal, 25 to 30 millimeters long and 7 square millimeters in diameter, is responsible for receiving the sound waves from the ear to the eardrum. When the tympanic membrane rumbles by these waves, specialized cell bodies interpret the sound.
The fungi that live in the hearing system are commensal and saprophytic, that is, they live normally in the otic flora and do not usually cause problems. In addition, cerumen has antifungal, bacteriostatic and hydrophobic properties, as indicated by studies from the Dialnet portal. For all these reasons, commensal mushrooms do not tend to overgrow.
Unfortunately, when certain environmental or internal imbalances arise, fungal populations can proliferate in the ear. Some of them synthesize toxins that damage tissues (such as Aspergillus), while others feed on skin keratin, such as dermatophyte fungi.
Symptoms
Bacterial external otic infection usually presents with pain and purulent discharge. This is not the case for otomycosis, as the clinical signs are nonspecific and generally less severe.
According to the Journal of Biological Diagnosis, the most common symptom in all cases is pruritus (itching). The patient also experiences ongoing discomfort, pain (sometimes not), hearing loss, and a feeling that the ear is “full.” These pictures are not usually accompanied by fever, nor does the posterior pinna become inflamed.
Furthermore, as the MSD Manual indicates, the infection can be seen with the naked eye. If the condition is caused by A. niger, gray spots (conidiophores) surrounded by velvety material (hyphae) appear in the ear canal. Infection with C. albicans is less visible, but usually causes a thick exudate that contains spores.
Causes and risk factors
Most of the fungi that cause otomycosis are saprophytes, that is, they feed on the waste substances that are present in the environment. In the case of humans, these microorganisms take advantage of the skin flakes and exudates to nourish themselves, without causing any damage.
However, there are certain factors that can cause an imbalance in fungal populations. Among them, we highlight the following:
- Environmental changes: a saprophytic fungus can become pathogenic if the conditions are right. High humidity and temperature promote fungal growth.
- Changes in the epithelium of the ear canal: for example, variations in the pH of the inner medium of the ear can facilitate infectious events.
- Changes in earwax: bathing in the usual way in the sea or practicing swimming facilitates the entry of water into the outer ear, which destroys the wax. The Centers for Disease Control and Prevention (CDC) makes links between swimming and ear infections.
- Immunosuppression: If there’s damage to the immune system, it is more possible for commensal species in the human body to develop uncontrollably. AIDS patients have these problems in the usual way.
- Abnormalities in the ear canal: if the person has previous injuries or irregularities, it is easier for the fungi to settle.
- Condition and social habits: curiously, wearing certain clothes that cover the ears (veils, earmuffs or sound insulators) could favor the appearance of otomycosis. The less contact the ear has with the medium, the more moisture accumulates, which facilitates fungal growth.
In summary, many factors can predispose to otomycosis, but environmental variations and water sports are usually the most common. Because antiretroviral therapy (ART) has slowed the severity of the condition of HIV-positive patients, it is no longer so common for them to develop fungal infections from commensal agents.
How to diagnose it?
As indicated by the Navarra University Clinic (CUN), external otitis is diagnosed with observation and physical examination. Through the use of an otoscope (medical instrument with a beam of light), the professional will be able to detect any abnormality seated in the external auditory canal.
Sometimes a culture of the patient’s ear epithelium exudate may be required under laboratory conditions. Applying antibiotics to a person infected with Aspergillus is useless, so you have to make sure that the diagnosed pathogen is correct. For fungi to grow, culture media are used.
As we have said, the treatment of choice is, in all cases, an antifungal. Some patients with otomycosis go to the specialist on successive occasions, due to wrong antibiotics and the infection progresses. Taking an antibiotic for a fungal infection is useless.
The medical journal International Archieves of Otorhinolaringology details the most common treatments in these cases. Antifungals, which you apply as drops in the ear, include the following:
- From the azole group (imidazole, miconazole, clotrimazole, etc.).
- Amphotericin B.
- Boric acid.
- Mercurochrome (1-2% solution).
- Phenylmercury acetate.
People use azole antifungals most commonly in almost all cases. These prevent the synthesis of ergosterol (the main component of the membranes of fungi), which prevents them from growing and reproducing in the tissue. You should not make the solutions with the antifungals if the eardrum is perforated, as they can damage structures.
Beyond this, over-the-counter pain relievers and antihistamines may also help, in order to reduce inflammation, itching, and pain. With the appropriate treatment in each case, the infection should subside in a few days without major complications.
Prevention and recommendations
A patient with a depressed immune system cannot avoid immunosuppression without pharmacological agents. So in these cases the only possible prevention is to put yourself in the hands of a professional. On the other hand, people in good health can avoid an otomycosis without resorting to medication, as long as they pay attention in certain areas.
For example, you have to be very careful when playing sports in the pool. Residual water can destroy earwax and unbalance the pH of the ear canal. Wear a bathing cap, and tilt your head well to the sides once you finish the activity. That way, you’ll to expel the water residues.
On the other hand, it should also be noted that cleaning your ears is good, but not excessively. It is not always appropriate to get rid of all the earwax from the ear canal. That’s because it has protective properties. Under no circumstances use swabs, as these only cause the accumulation of wax and contaminated matter in the ear.
Finally, let your ears “air” from time to time if you wear clothing or accessories that cover the pinna. The more moisture that accumulates in the ear canal, the more likely it is that commensal fungi will begin to multiply uncontrollably.
What is there to remember?
Otomycosis is not a serious infection in itself, but it can cause a lot of discomfort in the short term. To some extent, this picture can be avoided, but in other cases it is almost impossible. For example, you live in a region with very high humidity and high temperatures. Then, you can do little more than keep hygiene up to date.
If you have an earache for more than a couple of days, see your primary care doctor soon. An early diagnosis will prevent the pathology from worsening and affecting nearby areas, such as the inner ear.
Don’t forget to SHARE everything you know about this ear infection with your friends and family on your social networks!