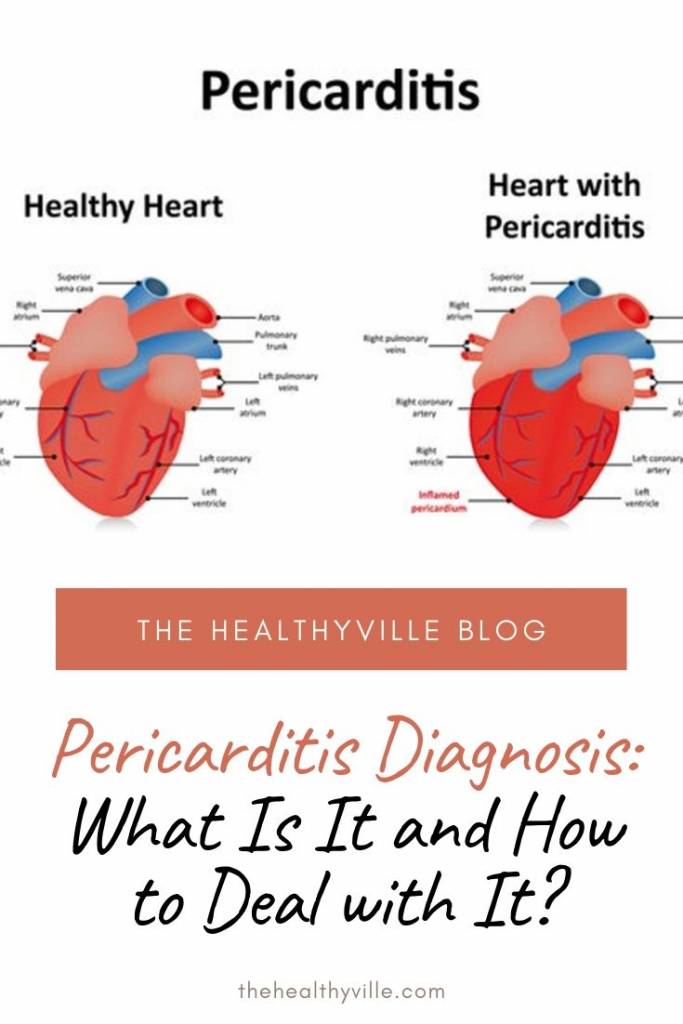
If you’ve got pericarditis diagnosis, you better be familiar with and learn how to deal with it. We have provided that info to you. It can save your life!
The symptoms of pericarditis are very similar to those of a heart attack. However, in a large number of cases, this problem resolves on its own and only requires common analgesics. Only rarely does it require larger measures.
Pericarditis is the inflammation of the pericardium. The pericardium, in turn, is a sac-shaped membrane that surrounds the heart. This membrane has two layers and between them there is a small volume of liquid, which serves as a lubricant and causes the two layers to slide between them, without causing problems.
When pericarditis occurs, the volume of the fluid increases. That can end up clogging the heart, preventing its functioning. However, in most cases there are no major problems and improvement without the need for treatment. The most serious cases require medication and only rarely, surgery.
Pericarditis mainly affects men between 20 and 50 years of age. In cases where it is impossible to treat it, the pericardium can be removed without causing consequences of consideration.
Types of pericarditis
Basically, there are two types of pericarditis: acute and chronic. Let’s see the characteristics of each of them:
Acute pericarditis It is characterized by its sudden onset. It lasts less than six weeks and, with relative frequency, generates pericardial effusions. The symptoms you experience are similar to those of a heart attack. Only a small percentage of patients have relapses.
Chronic pericarditis It arises as a result of a thickening of the pericardium or an accumulation of fluid. It lasts more than six weeks and can cause right ventricular failure, that is, edema in the abdominal area, pretibial area and ankles.
Chronic pericarditis occurs when a fibrous tissue is formed around the heart. This tissue compresses that organ and increases the pressure in the veins that carry blood to it. This causes the pericardium fluid to stagnate and, in its attempt to exit, end up accumulating in other parts of the body.
Causes
In 80% of cases it is impossible to establish the cause of pericarditis. However, it is very common that its origin is associated with some type of infection. The most common is that it is a viral infection. To a lesser extent, there is a base bacterial infection and only very rarely is it a fungal infection.
Likewise, there are many cases in which pericarditis appears associated with any of the following diseases:
- Autoimmune diseases.
- Cancer, including leukemia.
- AIDS.
- Renal insufficiency.
- Hypothyroidism.
- Tuberculosis.
- Rheumatic fever.
In other cases, the immediate history is a heart attack or cardiac surgery, as well as trauma to the thoracic area. Sometimes, pericarditis is related to an inflammation of the myocardium, the practice of radiotherapy in the chest or the use of some drugs.
Symptoms
The typical symptom of acute pericarditis is severe and stabbing pain in the chest area. It sits on the left side and behind the sternum. However, there are also many people who only experience mild and constant pain. Others report feeling a pressure in the chest, with a variable intensity.
Many times, pain is also felt in the left shoulder and neck. The discomfort becomes more intense at the time of coughing, inhaling deeply or at bedtime. Instead, he manages to dilute himself a little while sitting and lean forward somewhat.
In chronic pericarditis, chest pain is also usually the predominant symptom. In addition, both this and acute symptoms may appear as:
- Heart palpitations.
- Slight fever.
- Cough.
- Swelling in the legs.
- Feeling dizzy.
- Sickness.
- Weakness.
- Fatigue.
Pericarditis diagnosis and treatment
The milder cases of pericarditis usually resolve on their own. However, once you get pericarditis diagnosis, most of the time you’ll need to start a drug treatment. Usually, your doctor will prescribe the most common pain relievers to manage pain and reduce inflammation.
It is also possible that you get Colchicine, which reduces inflammation and prevents recurrent episodes. However, this drug is not safe for those suffering from liver or kidney disease, or for those taking certain medications.
When there is no response to these drugs, the measure to follow is usually to order corticosteroids. If the cause of pericarditis is a bacterial infection, doctors usually prescribe antibiotics prescribed to treat it.
In the most severe cases, especially if there is a suspicion of cardiac tamponade, it is appropriate to drain, by a pericardiocentesis procedure. It is rarely necessary to go to pericardiectomy, or definitive removal of the pericardium.
Don’t forget to SHARE all the info about pericarditis diagnosis with your friends and family on your social networks!